I’m not feeling great today, maybe I should skip the party…
“Hey, Jen! Are you coming?”
“No, I think I’m going to stay in.”
Later that night, you find yourself thinking, I’m such a failure, I’m so useless, I couldn’t even get to the party… And I’m not any kind of company right now…
When you have depression, it is absolutely exhausting. A big part of that is because it seems like this sick, endless loop. Like you’ve been cursed to listen to your least favourite song on repeat for the remainder of eternity.
People with depression often become progressively withdrawn over the course of their illness. Often times, people with depression will skip events because they feel like they are incapable of having fun. They may worry about ruining others’ evenings. In the immediacy, this strategy seems like the only tolerable option. In the long-term, social withdrawal, caused by depression, also exacerbates depression, which in turn leads to further avoidance.
These cycles of thinking and behaviour are well recognized in the field of psychiatry, and we utilize our understanding of this phenomenon to guide our treatments.
In broad strokes, psychiatric illnesses have two main modalities of treatment – medication and therapy based. They often work best in conjunction with each other. Today, I’ll be discussing cyclical behaviours and the role of cognitive behavioural therapy in the treatment of depression.
Cognitive behavioural therapy (CBT) is a manualized, evidence-based treatment for anxiety and depression. What does manualized mean? Don’t think of a guy on his couch discussing his relationship with his mother; that would be an open-ended psychotherapy, such as psychodynamic therapy. CBT is very specific, with worksheets, homework, and goals that are worked on by you and your therapist over a course of 2-4 months.
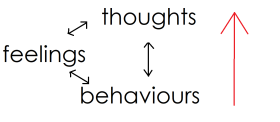
 CBT relies on a principle – that our thoughts, feelings, and behaviours are all related and that they inform each other. And this relationship is a two way street, Your thoughts inform your actions, and your actions inform your thoughts. Your feelings inform your actions and behaviours, and vice versa. I could go on.
CBT relies on a principle – that our thoughts, feelings, and behaviours are all related and that they inform each other. And this relationship is a two way street, Your thoughts inform your actions, and your actions inform your thoughts. Your feelings inform your actions and behaviours, and vice versa. I could go on.
In CBT, you and your therapist will work together to address all three of these elements simultaneously. Thought records and your time with your therapist are used to explore thoughts and feelings, and to understand how behaviours may have an impact on how you feel. Remember the cycle of depression and social avoidance.
 Over time, you and your therapist hope to achieve cognitive restructuring – literally a change in the way you think. Instead of thinking, “I’m too tired for that party,” you might find yourself thinking, “I’m tired and I should go to the party for at least a few minutes – it will probably be fun.” Cognitive restructuring takes time, and considerable investment. It can be considered the “top down approach,” because it focuses on thoughts/the brain/the “top.”
Over time, you and your therapist hope to achieve cognitive restructuring – literally a change in the way you think. Instead of thinking, “I’m too tired for that party,” you might find yourself thinking, “I’m tired and I should go to the party for at least a few minutes – it will probably be fun.” Cognitive restructuring takes time, and considerable investment. It can be considered the “top down approach,” because it focuses on thoughts/the brain/the “top.”
A big – and underappreciated – aspect of CBT is behavioural activation, or the “bottom up approach.” When you’re depressed, and have been withdrawn for some time, it literally becomes difficult to have a positive thought. It also becomes easier to have negative thoughts, and you lose enjoyment in things you had previously found enjoyable. This isn’t just partying and socializing, but also things like laundry, and brushing your teeth, things that previously resulted in satisfaction but now seem insurmountable.
 Behavioural activation acknowledges this disconnect and works to encourage people to do things anyway, despite the sense that no enjoyment or satisfaction will be wrought. Behavioural activation “kick starts” our brain, and gives us the ability to feel positive about things again. This can in turn make the cognitive restructuring arm of CBT a little easier, and before you know it, the cycle is working in the opposite direction, and improving your mood.
Behavioural activation acknowledges this disconnect and works to encourage people to do things anyway, despite the sense that no enjoyment or satisfaction will be wrought. Behavioural activation “kick starts” our brain, and gives us the ability to feel positive about things again. This can in turn make the cognitive restructuring arm of CBT a little easier, and before you know it, the cycle is working in the opposite direction, and improving your mood.
When I work on behavioural activation with patients, we often start with simple things such as brushing your teeth, or making your bed in the morning. We escalate the therapy progressively, and before you know it, the most out of reach goals are within the patients grasp.
I know when I started my residency, therapy seemed like a bit of an enigma. Now, I have a bit of an understanding, and it has empowered me. I hope I have been able to empower you!
Dr. Travis Barron is a resident physician in Toronto, Canada.

Cognitive restructuring is vitally important. Many people have faulty thinking patterns. These patterns are learned, often from parents who had the same patterns. Faulty thinking patterns , which often lead to anxiety and depression, can also be unlearned.
Thanks for sharing.
LikeLiked by 1 person
Thanks for the comment!
LikeLiked by 1 person
I have mixed feelings about this. From a professional standpoint, I’m quite pro-CBT. From a personal perspective, I’ve seen its limitations. In the past I’ve tried to persist with physical activity and socialization and stuck with it for months, but I didn’t get any better and if anything those things only became more aversive. Now I’m just a lot more selective when it comes to activation.
LikeLiked by 1 person
Well said! There is no one-size-fits-all approwch
LikeLiked by 1 person
Great post thank you
Can you share your opinion on the merging of cbt with mindfulness
Therapies have proliferated now but ACT and DBT were the originals
And another question I have, how important is it for your Clint’s to work in healing between sessions?
LikeLike
Thanks for the comment!
CBT, DBT, mindfulness, are all different therapy modalities. They can often complement one another. It’s unusual for certain therapies to be mixed -CBT and DBT for example, are often indicated for different illnesses (Depression/Anxiety vs personality disorders).
CBT and mindfulness do compliment each other, but by no means is it make orr break depending on which therapy (or both) you an enrolled in. CBT has evidence for treating an acute depressive episode, Mindfullness actually has evidence that it can prevent further episodes! So basically I recommend it to everyone, when it’s available, which is not very often.
CBT will not work unless the client is working in between sessions. The majority of the work is done by the client in the down time; the therapy sessions serve as more of a guide!
Hope this helps.
LikeLiked by 1 person
I totally agree. Daily work in healing helps tremendously
I run a mindfulness group and it is extremely difficult to change a disorder or even behavior.
It is the exception that someone understates a daily practice of 15 minutes.
I believe one of your most important skills is the ability to inspire a client to take action.
LikeLiked by 1 person
On point, my friend!
LikeLike
wow these are good to know information. Last time I read something about these therapies – it’s been way back in college. Thank you for sharing your in depth knowledge about behavioral therapy. Having a better understanding is always good.
LikeLiked by 1 person
Very informative post! My step-daughter has severe depression and will have her subscribe to your blog. Thank you so much for all you do! Great post!
LikeLiked by 1 person
Thank you! Best wishes to her
LikeLike
Just as I read this post I realized that I am depressed and not just anxious. Sometimes you have to see it in black and white. I have Parasesthia and have tapered off Prozac to see if that is the culprit. Bloody mental health!!
LikeLike
I’m glad to share some clarity! If you have diagnostic doubts I’d see your doctor. These thinking loops are also common in anxiety! Doctors are often helpful.
LikeLiked by 1 person
I see my psychiatrist every three months, so I am fortunate. Thank you.
LikeLike